Understanding Endometriosis
Reliable information and support for those affected by endometriosis
What is Endometriosis
Endometriosis is a chronic condition in which tissue similar to the lining of the womb (endometrium) grows outside the uterus. These deposits most commonly affect the ovaries, fallopian tubes, pelvic lining, bowel, and bladder.
Each month, this tissue responds to hormonal changes, which can lead to inflammation, scarring, and adhesions. Over time, this may cause persistent pelvic pain and affect fertility.
Endometriosis affects approximately 1 in 10 women of reproductive age, although the severity of symptoms varies significantly between individuals.


Types of Endometriosis
Peritoneal endometriosis is the most common form of endometriosis.
It occurs on the pelvic peritoneum, which is a thin membrane lining the inside of the pelvis and covering the pelvic organs.
In this type:
Lesions are usually small and shallow
They sit on the surface of pelvic structures
Despite being superficial, they can still cause significant pain and inflammation
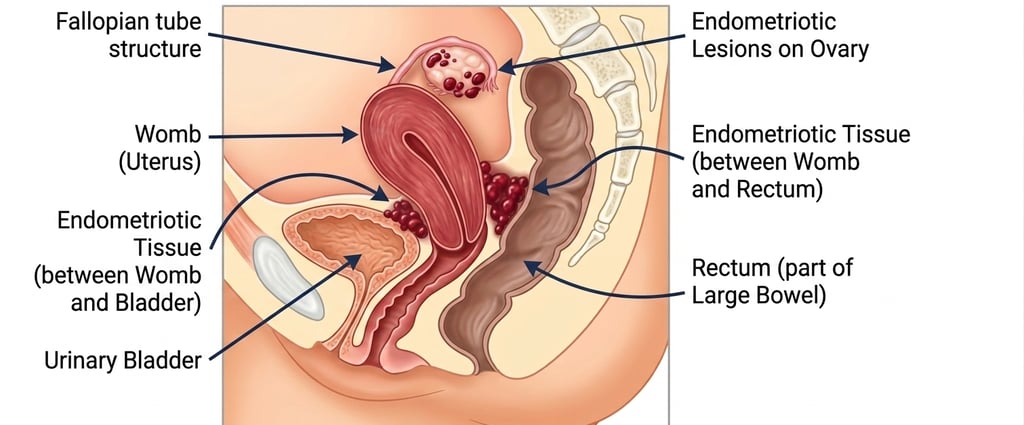
Peritoneal (Superficial) Endometriosis
Ovarian Endometriosis (Endometrioma)
Ovarian endometriosis, also known as an endometrioma, occurs when cysts form within the ovaries.
These cysts are sometimes referred to as:
“Chocolate cysts”, because they contain old, dark blood
In this type:
Cysts develop inside one or both ovaries
They may affect ovarian function
They can be associated with pelvic pain and subfertility
Deep endometriosis occurs when lesions grow deeper beneath the surface, often affecting surrounding organs.
Common sites include:
The bowel
The bladder
The recto-vaginal septum (the tissue between the vagina and rectum)
In this type:
Lesions penetrate more than 5 mm beneath the surface
It is often associated with more severe symptoms
It may cause pain during bowel movements, urination, or intercourse
Deep Infiltrating Endometriosis (Deep Endometriosis)
Extra-pelvic endometriosis occurs when endometriosis develops outside the pelvis.
Although less common, it can affect areas such as:
The thorax (chest)
Caesarean section scars
Other distant parts of the body
Symptoms depend on the location of the disease and may sometimes occur in a cyclical pattern related to the menstrual cycle.
Extra-Pelvic Endometriosis
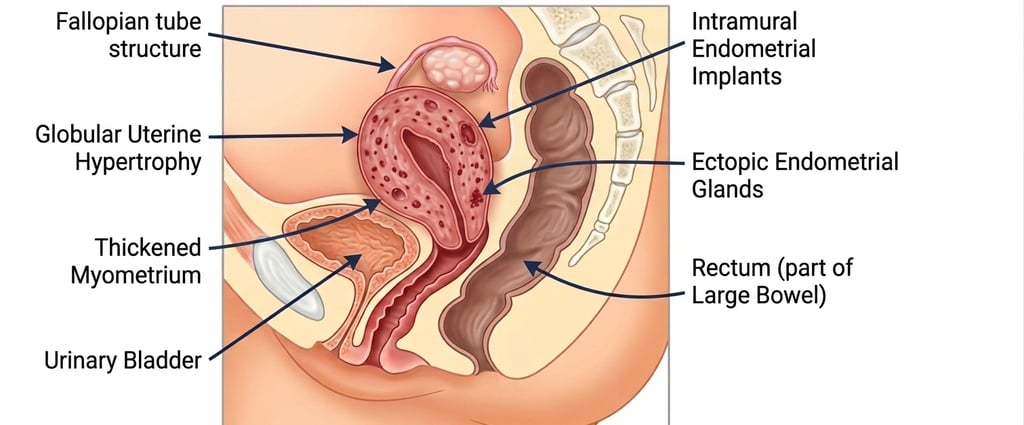
Adenomyosis
A closely related condition is adenomyosis.
This occurs when cells similar to those lining the womb grow within the muscle wall of the womb.
Key points about adenomyosis:
It responds to hormonal changes during the menstrual cycle
It affects approximately 1 in 10 women
It commonly causes:
Heavy menstrual bleeding
Painful periods
Pelvic discomfort
It is possible to have:
Endometriosis alone
Adenomyosis alone
Both conditions together, which is relatively common
Common Symptoms of Endometriosis
Symptoms can vary widely, and some women may have severe disease with minimal symptoms, while others experience significant pain.
Common symptoms include:
Severe period pain (dysmenorrhoea)
Chronic pelvic pain
Pain during sexual intercourse (dyspareunia)
Pain when opening bowels, especially during periods
Pain when passing urine
Heavy periods
Fatigue
Infertility or difficulty conceiving
Bloating, sometimes referred to as “endo belly”
Symptoms often worsen over time if untreated.
When Should You Seek Medical Advice?
You should consider seeing a specialist if:
Period pain interferes with daily activities
Pain is worsening over time
Painkillers are no longer effective
You have difficulty conceiving
You experience bowel or bladder symptoms during periods
Symptoms persist despite treatment
Early diagnosis may help reduce long-term complications.
Causes of Endometriosis
The exact cause of endometriosis remains unclear, but several theories exist.
Possible contributing factors include:
Retrograde menstruation
Genetic predisposition
Immune system dysfunction
Hormonal influences
Surgical scar implantation (rare)
Women with a family history of endometriosis may have a higher risk.
How is Endometriosis Diagnosed?
Diagnosis begins with a detailed clinical history and physical examination.
Investigations may include:
Ultrasound Scan
A specialist pelvic ultrasound can detect:
Endometriomas (ovarian cysts caused by endometriosis)
Deep infiltrating endometriosis
Adhesions
MRI Scan
MRI may be recommended for:
Deep endometriosis
Bowel or bladder involvement
Surgical planning
Laparoscopy
Laparoscopy is considered the gold standard for diagnosing endometriosis. This is a minimally invasive surgical procedure performed under general anaesthetic, allowing direct visualisation and treatment of disease.
Treatment Options for Endometriosis
Treatment depends on:
Symptom severity
Age
Fertility plans
Disease extent
Previous treatments
Management usually involves medical therapy, surgery, or a combination of both.
Medical Treatment
Medical treatment aims to control symptoms and suppress disease progression.
Options may include:
Hormonal contraception (combined pill or progesterone-only methods)
Hormonal intrauterine system (coil)
GnRH analogues
Pain management medications
These treatments may reduce symptoms but do not remove disease tissue.
Surgical Treatment
Surgery is recommended in selected cases, particularly where symptoms are severe or fertility is affected.
Procedures may include:
Laparoscopic excision of endometriosis
Removal of ovarian endometriomas
Treatment of adhesions
Treatment of bowel or bladder involvement (in advanced disease)
Excision surgery performed by an experienced specialist is associated with improved symptom relief.
Endometriosis and Fertility
Endometriosis may affect fertility through:
Adhesions affecting fallopian tubes
Ovarian cysts
Inflammation within the pelvis
However, many women with endometriosis conceive naturally.
Fertility options may include:
Ovulation monitoring
Surgical treatment
Assisted reproductive techniques
Management should be individualised.
Living with Endometriosis
Long-term management may include:
Pain management strategies
Hormonal suppression
Lifestyle support
Multidisciplinary care when required
Regular follow-up helps monitor symptoms and treatment effectiveness.
When to Seek Urgent Medical Advice
Seek urgent medical attention if you experience:
Severe sudden pelvic pain
Fever with pelvic pain
Persistent vomiting
Symptoms of bowel obstruction
Severe bleedingx
FAQs
Can endometriosis be cured?
There is currently no permanent cure, but treatments can effectively control symptoms and improve quality of life.
Can endometriosis return after surgery?
Why Choose Specialist Care?
Can endometriosis cause cancer?
Does pregnancy cure endometriosis?
Endometriosis is a complex condition that often requires expert assessment and individualised treatment planning.
Specialist care ensures:
Accurate diagnosis
Individualised treatment
Advanced surgical options when required
Fertility-focused management
Multidisciplinary support when needed
Pregnancy may temporarily improve symptoms, but it does not cure the condition.
Recurrence is possible, particularly without hormonal suppression following surgery.
Endometriosis is a benign condition. The risk of cancer is very low.
More resources
Provide a general summary of the services you provide, highlighting key features and benefits for potential clients.






This patient guide helped me understand my symptoms and feel less alone in my endometriosis journey.
Anna K

★★★★★
Contact
Reach us Monday to Friday, 9am to 5pm
Phone
+447928306699
Gynaescope LTD© 2026. All rights reserved.
